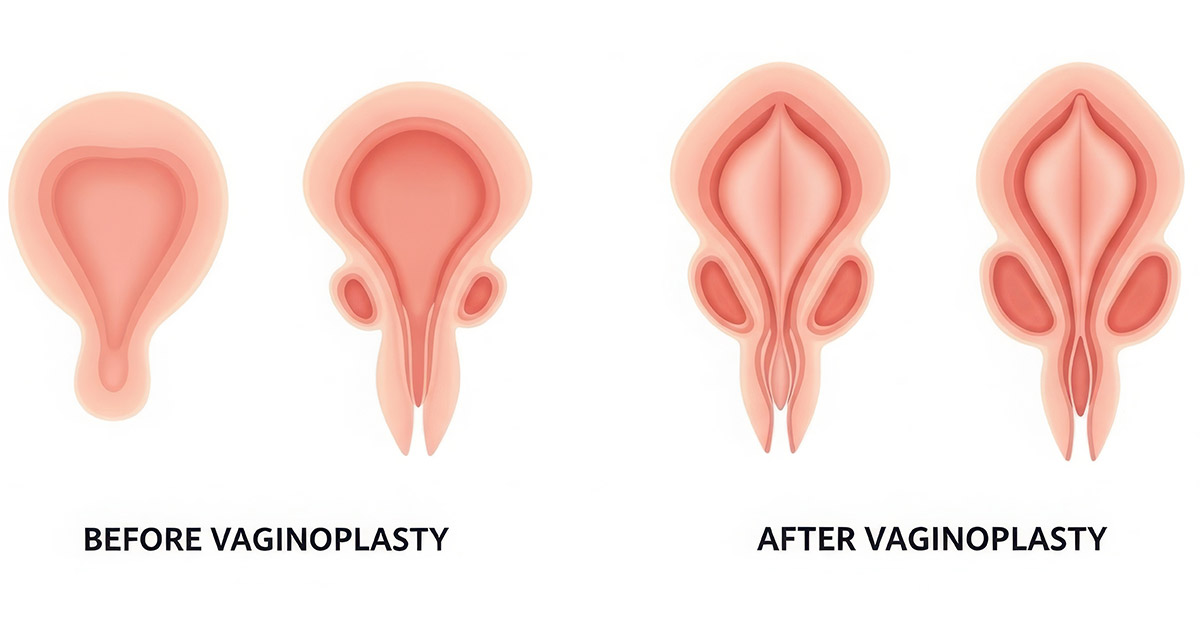
Vaginoplasty for vaginal rejuvenation is a functional and aesthetic procedure designed to restore vaginal tightness, improve pelvic floor support, and enhance sexual comfort following childbirth, aging, or tissue laxity. Understanding what a healed vaginoplasty looks like helps women form realistic expectations and recognize normal healing milestones.
This article provides a detailed, science-informed overview of postoperative tissue remodeling, scar maturation, and long-term aesthetic and functional outcomes.
Understanding Vaginoplasty For Vaginal Rejuvenation
Vaginoplasty involves surgically tightening and re-supporting the vaginal canal by approximating the levator ani muscles and excising redundant mucosa. Some procedures include perineoplasty, which refines the opening of the vaginal introitus and reconstructs the perineal body. The goal is to restore structural integrity, improve sensation, and create a more youthful anatomic appearance. The healed outcome of vaginoplasty surgery depends on the precision of muscle plication, mucosal closure, and the patient’s healing physiology.
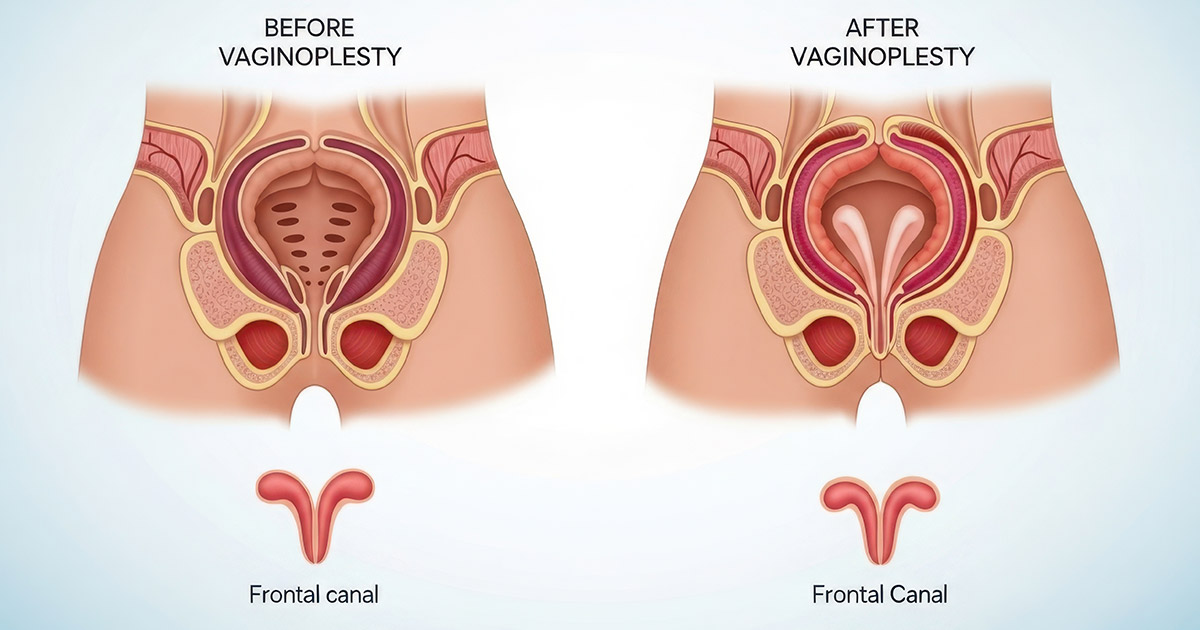
Unlike non-surgical technologies that rely on thermal collagen remodeling, surgical vaginoplasty produces predictable and longer-lasting tightening because it physically reduces tissue laxity and reconstructs muscular support1.
The Vaginoplasty Recovery Timeline and Healing Phases
The vaginoplasty recovery timeline typically spans 12 weeks, with deeper collagen maturation continuing for several months. Each phase corresponds to distinct biological processes such as inflammation, fibroblast activity, angiogenesis, and epithelial remodeling.
First Week
Swelling, bruising, and tenderness are expected due to fluid accumulation and early inflammatory response. Sutures may be visible externally, and tissue coloration can appear bright red or purplish due to increased blood flow. None of these features reflects the final healing.
Weeks Two to Four
Swelling begins to reduce as lymphatic drainage improves. Dissolvable sutures soften and shed. Patients may feel tightness as collagen deposition intensifies. Externally, the perineum starts to appear smoother and less swollen. Internal mucosa regains uniform texture as epithelial cells regenerate.
Weeks Four to Eight
Most significant swelling subsides, and the surgical site begins to resemble a more stable configuration. Scars lighten considerably. At this stage, women often begin to notice early healed vaginoplasty results, although structural remodeling is still ongoing.
Weeks Eight to Twelve
This period is critical for determining what a fully healed vaginoplasty will look like. Scar tissue undergoes reorganization as collagen fibers arrange into stronger, more elastic patterns. Patients are usually cleared for intercourse at this time, and many describe improved tightness and comfort, contributing to a functional understanding of sex after vaginoplasty.
Three to Twelve Months
Long-term refinement occurs as scar tissue becomes flatter and paler. Mucosa thickens, and normal sensation continues to recover as nerve endings regenerate.
What a Fully Healed Vaginoplasty Looks Like
A fully healed vaginoplasty has distinct features, both externally and internally, reflecting completed tissue repair and scar maturation.
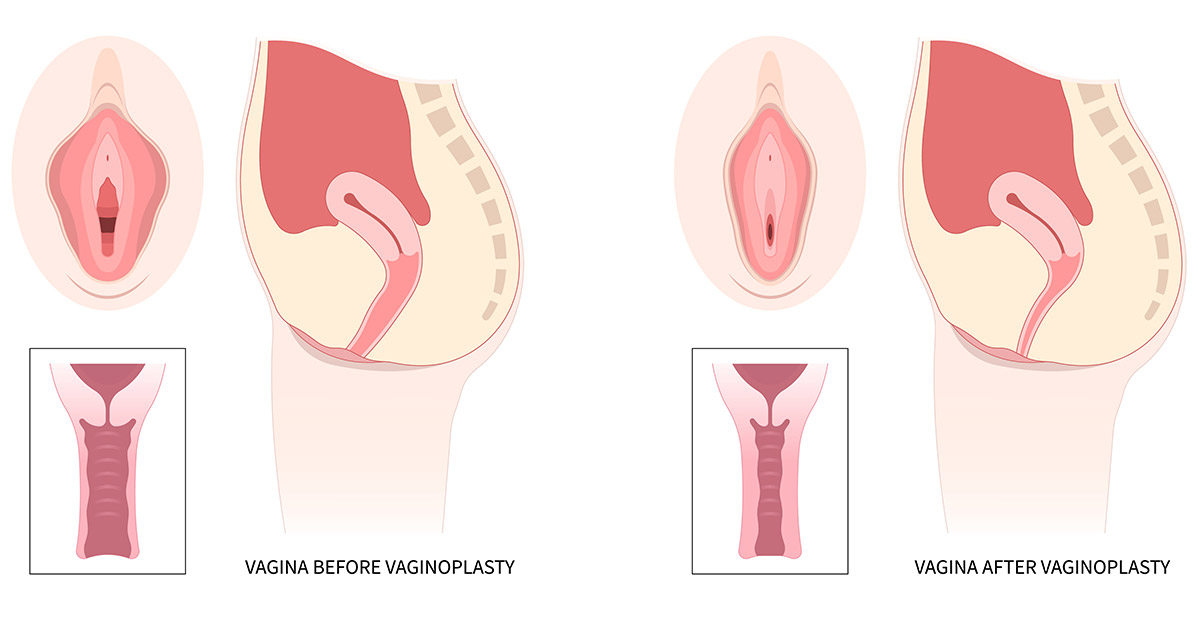
External Appearance
A typical post-op healed vaginoplasty perineum appears smooth, symmetrical, and free of visible suture marks. Incisions are strategically placed in natural creases, leading to thin, pale scars that are usually difficult to distinguish from surrounding tissue. The introitus often appears more defined and supported, with restored perineal body height, which contributes to vaginal firmness.
The labia minora and majora maintain their natural anatomy unless adjunctive procedures are performed. Minor variations in coloration are normal and related to vascular remodeling.
Internal Appearance
A healed vaginoplasty internally reveals a tighter, uniformly toned vaginal canal. The mucosa appears pink, moist, and healthy due to restored epithelial integrity. Rejuvenation typically resolves preoperative issues like laxity or gaping. Studies show that levator ani muscle plication significantly improves vaginal support and functional outcomes, directly influencing the internal appearance and feel of a vaginoplasty surgery healed state2.
Functional Outcomes
After a fully healed vaginoplasty, most women report improved sexual sensation, enhanced friction, and decreased feelings of looseness. Pelvic stability and urinary control may also improve depending on the preoperative condition. These outcomes reflect restoration of tissue biomechanics and neuromuscular support.
How Scars Look When Vaginoplasty Is Fully Healed
Scar maturation is a critical determinant of healed vaginoplasty results. Internal scars are hidden and typically imperceptible within the mucosa. External scars fade over several months due to collagen remodeling and normalization of vascular supply. Thin, pale, flat scars are expected. Hypertrophic scarring or raised tissue is uncommon due to the high vascularity of the vulvar region, but may occur in patients with a genetic predisposition.
Indicators of Healthy Vaginoplasty Healing
Recognizing normal healing patterns helps differentiate expected changes from complications. Indicators include:
- Gradual reduction in swelling and improved tissue coloration
- Even epithelial coverage without open areas
- Restoration of symmetrical tissue contours
- Comfortable pressure sensation rather than sharp pain
- Absence of discharge, abnormal odor, or significant bleeding
- Progressive softening of scar tissue
These features are consistent with stable and healed vaginoplasty results.
When Healing Deviates From Normal
Signs that require evaluation include:
- Persistent severe pain or increasing redness
- Foul discharge or fever
- Separation of incision lines
- Thickened, raised, or painful scar tissue
- Painful intercourse after the typical healing window
- Visible asymmetry that worsens over time
These issues may reflect infection, dehiscence, or abnormal scarring and require attention from a surgeon.
Factors That Influence Vaginoplasty Healing Quality
Healing outcomes vary based on:
- Surgical precision and the method used to approximate muscles
- Patient age, hormonal status, and tissue elasticity
- Smoking, which decreases oxygen delivery and delays healing
- Postoperative compliance, including activity restrictions and hygiene
- Underlying medical conditions that impair microvascular circulation
Optimal vaginoplasty results require strict adherence to postoperative guidelines and avoidance of early strain on the surgical site.
FAQs About Vaginoplasty Healing
How long until vaginoplasty is fully healed?
Most women achieve a fully healed vaginoplasty between eight and twelve weeks, although deeper collagen remodeling continues for up to a year.
Will scars be visible to a partner?
External scars are typically subtle and fade well, while internal scars are not visible during intercourse. Partners usually notice functional improvements rather than residual scarring.
What does a healed result feel like during intercourse?
After a vaginoplasty surgery’s healed state, increased friction, enhanced tightness, and improved pelvic support are reported. Comfort typically improves due to stronger tissue integrity.
Can I expect my vagina to look completely different?
A healed vaginoplasty enhances firmness and symmetry but does not drastically alter natural anatomy. Normal variations remain, preserving individual appearance.
Understanding the Long-Term Appearance of Vaginoplasty
A fully healed vaginoplasty blends natural appearance with restored function. When performed by skilled surgeons and supported by proper postoperative care, the outcome includes well-healed tissues, improved tightness, and minimal scarring. Women considering the procedure can expect discreet, refined, and highly functional results once healing is complete.

At Alinea Labiaplasty & Vaginoplasty NJ, we offer advanced vaginoplasty and a range of effective vaginal rejuvenation procedures tailored to your anatomy, symptoms, and goals. Using evidence based techniques focused on both function and aesthetics, we help address vaginal laxity, discomfort, and sexual dysfunction safely and discreetly. If you are considering vaginoplasty or another vaginal rejuvenation treatment, contact our team to schedule a confidential consultation and receive a personalized treatment plan.
References
- İşlek Seçen E, Toksoz R. Impact of vaginoplasty on hiatal dimensions measured by translabial ultrasonography. Medicine. 2025;104:n. pag.
- Xu Y, Wei L, Liu M, et al. Transvaginal posterior levatorplasty and perineoplasty for female primary stress urinary incontinence: 12-month follow-up and technical presentation. BMC Urol. 2024;24(1):235. doi:10.1186/s12894-024-01604-7.